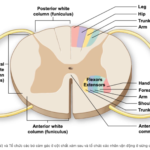
ANATOMY REVIEW
Bone and Joints
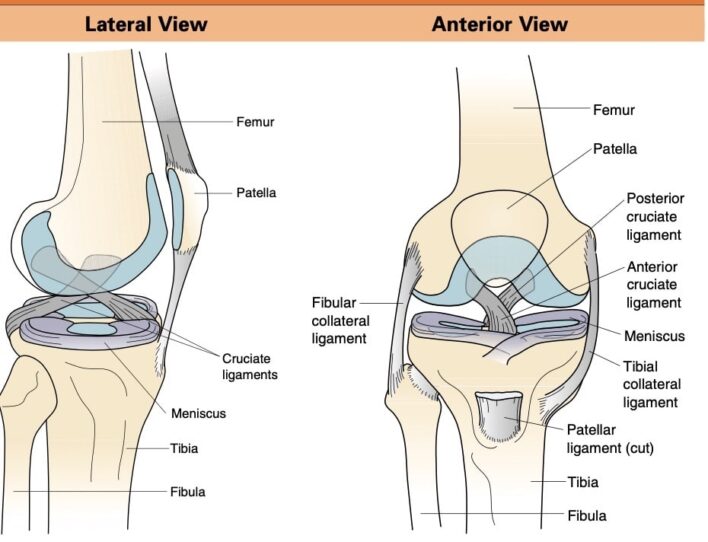
Terminology/Từ vựng:
- Knee: gối (genou)
- Femur: Xương đùi (femoral, adj)
- Tibia: Xương chày (tibial, adj)
- Fibula: Xương mác (fibular, adj)
- Patella: Xương bánh chè (patellar, adj)
- Meniscus: Sụn chêm
- Cruciate ligament: dây chằng chéo
- Anterior cruciate ligament: dây chằng chép trước, ACL
- Posterior cruciate ligament: dây chằng chéo sau, PCL
- Fibular collateral ligament: dây chằng bên mác = lateral collateral ligament: dây chằng bên ngoài
- Tibial collateral ligament: dây chằng bên chày – medial collateral ligament: dây chằng bên trong
Physiologic (Osteokinematic) Motions of the Knee
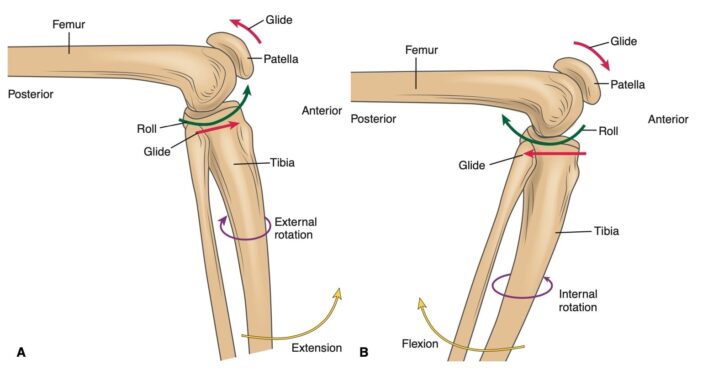
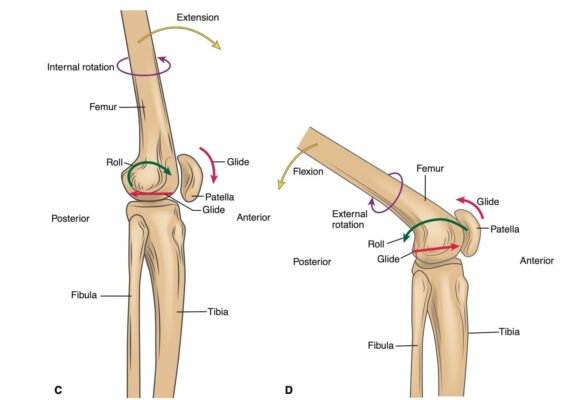
- Tibiofemoral (TF) joint: Khớp chày – đùi
- Patellafemoral (PF) joint: Khớp bánh chè – đùi
- Flex: gập/Ext: duỗi
- Abd: dạng/Add: khép
- IR (internal rotation): xoay trong
- ER (external rotation) xoay ngoài
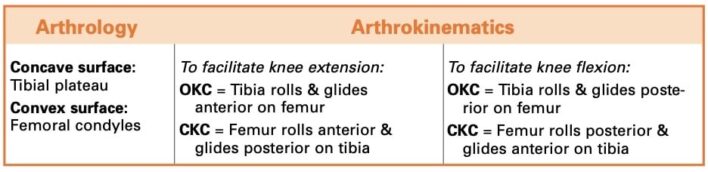
Accessory (Arthrokinematic) Motions of the Knee
Notes/Ghi chú:
- Physiologic Motions: vận động sinh lý, chuyển động xương
- Accessory Motions: vận động phụ trợ, chuyển động học khớp, joint play
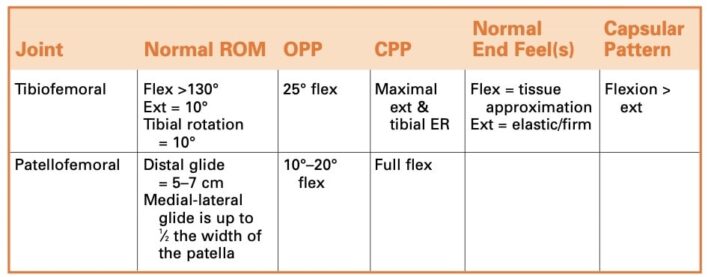
- OPP: Open Packed Position/ Tư thế khớp mở = resting position, tư thế khớp nghỉ: là tư thế thường dùng bắt đầu để di động khớp. Ghi nhớ quy luật mặt lồi/lõm
- CPP: Closed Packed Position/ Tư thế khớp khoá
- OKC: Open Kinetic Chain: Chuỗi động mở: Kỹ thuật di động khớp thường dùng ở chuỗi động mở để khu trú lên khớp được thực hiện
- Concave: lõm
- Convex: lồi
- Glide: trượt
- Distraction: kéo tách
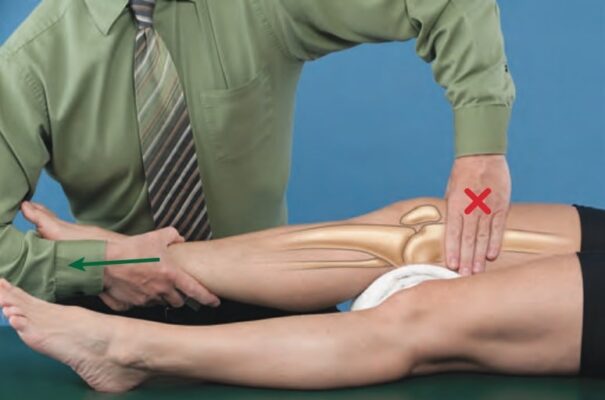
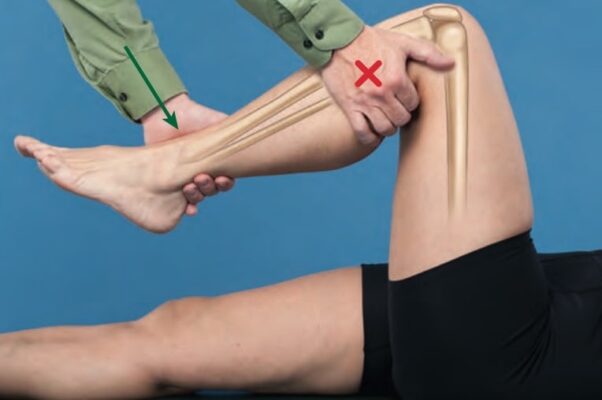
- Trong kỹ thuật, kỹ thuật viên thực hiện cố định đầu gần/phần xương cố định: Dấu chéo đỏ
- Kỹ thuật viên thực hiện vận động phụ trợ: Mũi tên xanh
- Người bệnh có thể thực hiện vận động sinh lý phối hợp: Mũi tên vàng
Lưu ý:
- Mâm chày lõm khớp với các lồi cầu xương đùi lồi.
- Tư thế nghỉ (OPP): Gối gập 25 ̊.
- Mặt phẳng điều trị: Mặt phẳng điều trị dọc theo bề mặt của mâm chày; do đó, nó di chuyển cùng với xương chày khi góc khớp gối thay đổi.
- Cố định. Trong hầu hết các trường hợp, xương đùi được cố định bằng đai hoặc bằng bàn điều trị.
PATELLOFEMORAL JOINT MOBILIZATIONS
Patellofemoral Glide and Tilt
Indications:
- Superior & inferior glide is to improve knee ext & flex, respectively
- Medial & lateral glide is to improve knee IR & ER, respectively
- Tilt is to improve all physiologic knee motions
Accessory Motion Technique
- Patient Position:
- Supine with knee in open-packed position.
- Clinician position & Hand Placement:
- Stands to side of pt
- Stabilization: Provided by the weight of the leg
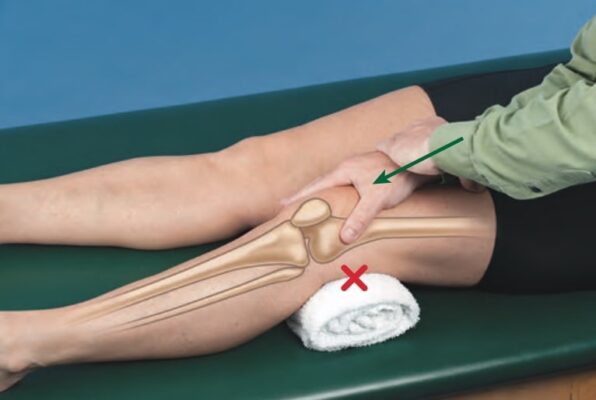
- Mobilizing hand: Patella is contacted with web space of hand
- Superior or inferior glide: hand placed at inferior or superior poles of patella, respectively
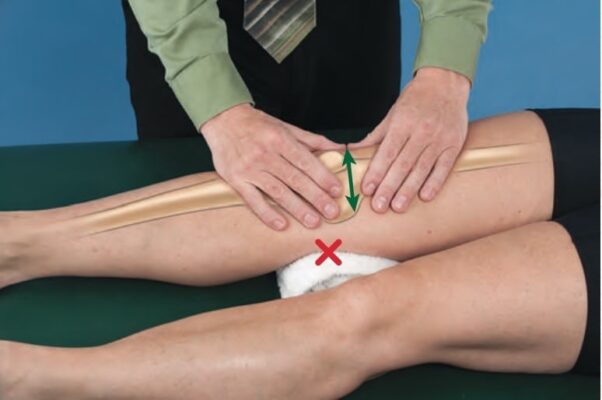
- Medial or lateral glide: hand placed at lateral or medial aspects of patella, respectively
- Tilt: thumbs placed over superior, inferior, medial, or lateral aspect of patella
- Force Application:
- For glides, your forearm is in line with the direction in which force is applied as your other hand provides reinforcement.
- For tilts, apply force in a posterior direction through the patellar contact with the objective of moving the opposing pole of the patella anteriorly.
Accessory With Physiologic Motion Technique
- Patient Position:
- The patient may be in an open chain sitting position or standing.
- Clinician position & Hand Placement:
- Utilize all hand contacts as described above.
- Force Application:
- Superior or inferior glides may be performed during open kinetic chain or closed kinetic chain active knee extension or flexion, respectively.
- Medial or lateral glides can be performed during closed kinetic chain tibial IR or ER, respectively, or during active knee extension and flexion. Mobilization force is maintained throughout the entire range of motion and sustained at end range.
TIBIOFEMORAL JOINT MOBILIZATIONS
Tibiofemoral Distraction
Indications:
- Testing; initial treatment; pain control; general mobility
Accessory Motion Technique
- Patient Position:
- Supine with the knee in the open-packed position or prone with the knee flexed to the point of the restriction
- Clinician position & Hand Placement:
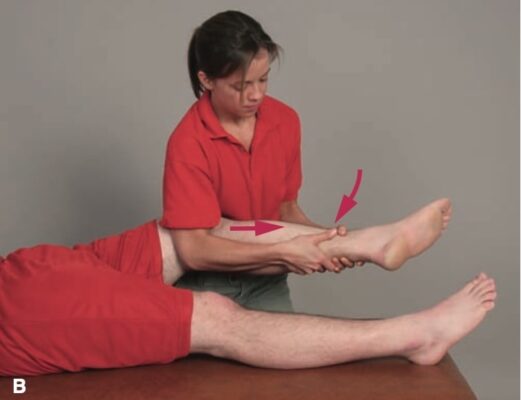
- Stands at foot of pt facing cephalad
- Stabilizing contact: In supine, distal thigh is stabilized over a bolster or mobilization straps can be used; in prone, stabilization provided through clinician’s elbow over posterior thigh
- Mobilizing contact: 1–2 hands grasp just proximal to ankle
- Force Application: Through your mobilization hand contact, apply a long-axis distraction force.
Accessory With Physiologic Motion Technique
- Patient Position:
- For knee extension, the patient is in a sitting position.
- For knee flexion, the patient is prone with the knee flexed to the point of restriction.
- Clinician position & Hand Placement:
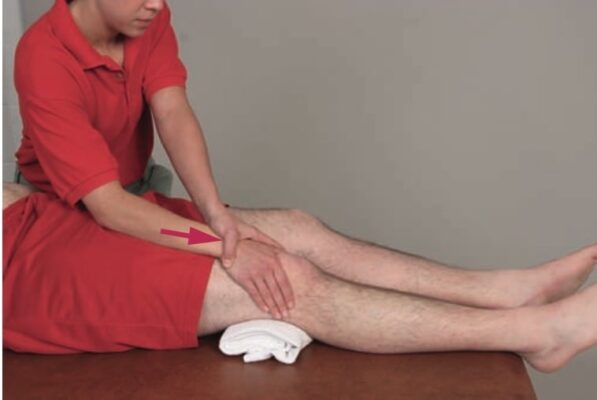
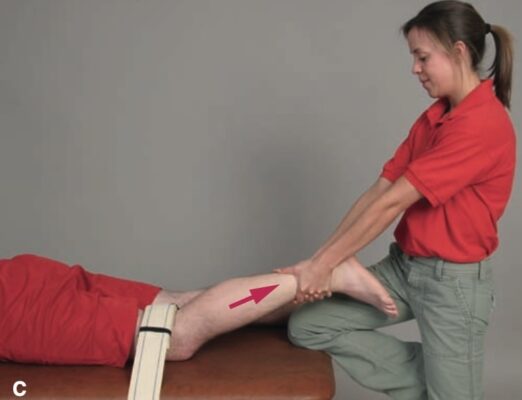
- For knee extension: Sit facing the patient. Provide stabilization at the patient’s anterior distal thigh. Grasp the lower leg just proximal to the ankle with your mobilization hand(s).
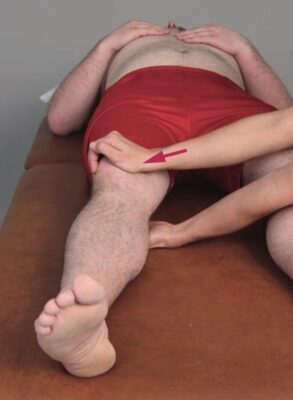
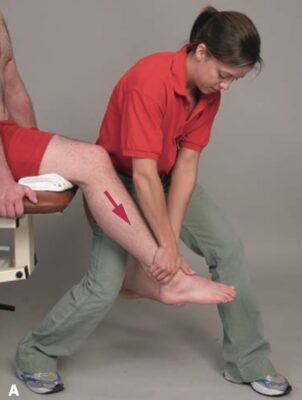
- For knee flexion: Stand on the side of the knee being mobilized. Place your elbow over the patient’s posterior thigh just proximal to the knee to provide stabilization. A towel may be used to improve patient comfort. Your clasped mobilization hands grasp the patient’s leg just proximal to the ankle.
- Force Application:
- For knee extension, apply a long axis distraction force through your mobilization hand contact as the patient actively moves into knee extension. Be prepared to move during motion in order to ensure that your forearm is in line with the direction in which force is applied.
- For knee flexion, maintain your mobilization hand contacts as the knee is passively flexed. As the length of the tibia effectively decreases relative to the length of your forearm, a distraction force is produced. There is no need to exert an additional distraction force during this procedure.
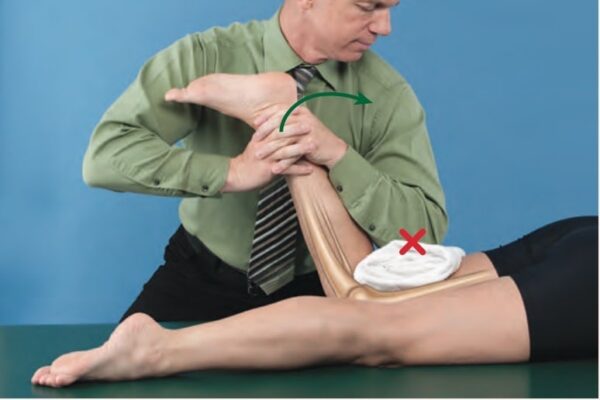
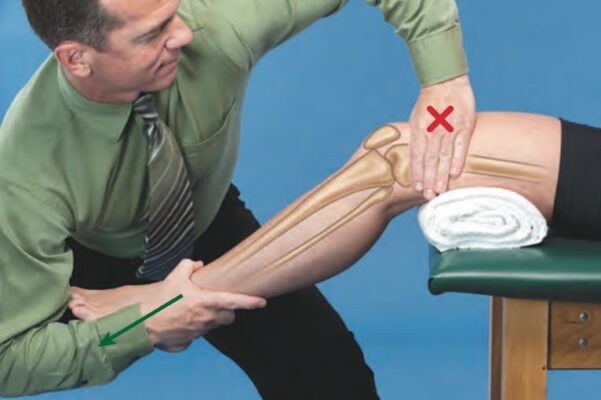
Tibiofemoral Anterior Glide
Indications:
- To improve knee ext
Accessory Motion Technique
- Patient Position:
- Prone with knee in open-packed position & bolster or wedge just proximal to knee to eliminate pressure on patella
- May be pre-positioned in varying degrees of flex to point of restriction with bolster under distal leg for support
- Clinician position & Hand Placement:
- Stands on ipsilateral side
- Technique 1: Prone
- Stabilizing contact: Just proximal to ankle providing counterforce to maintain knee position or stabilization provided by placing lower leg on clinician’s shoulder if knee is flexed >90°
- Mobilizing contact: Heel of hand contacts posterior aspect of proximal tibia just below knee with forearm in direction of force (may vary, depending on position of knee) or both hands contact proximal tibia if knee is flexed >90°
- Technique 2: Supine
- Stabilizing contact: Cephalad hand just proximal to anterior aspect of knee
- Mobilizing contact: Caudal hand scooped under posterior aspect of proximal tibia with forearm controlling distal tibia
- Force Application:
- Apply force through your mobilization hand contact in an anterior direction that is parallel to the treatment plane of the joint.
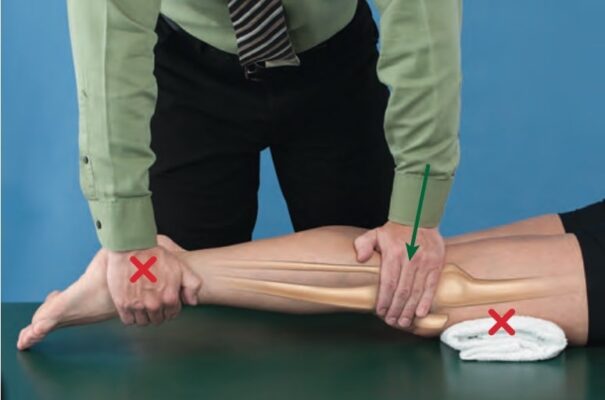
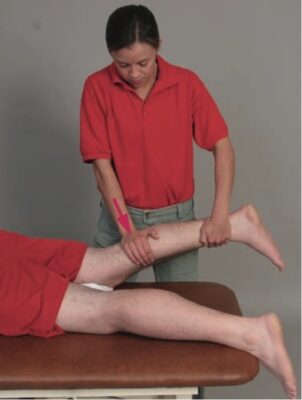
Accessory With Physiologic Motion Technique
- Patient Position:
- The patient is standing with the knees flexed in a squat position.
- Clinician position & Hand Placement:
- You are in a lunge position facing the patient.
- The mobilization belt is positioned over the posterior aspect of the patient’s proximal tibia and around your leg. One hand is used to reinforce the mobilization belt as the other hand assists in controlling motion into knee extension or both hands may be placed proximal to the knee anteriorly for stabilization.
- Force Application:
- The patient actively moves from a squat position into an erect standing position moving the knee into extension as you apply an anterior glide through the mobilization belt as the femur is stabilized.
- Mobilization force is maintained throughout the entire range of motion and sustained at end range.

Tibiofemoral Posterior Glide
Indications:
- To improve knee flex
Accessory Motion Technique
- Patient Position:
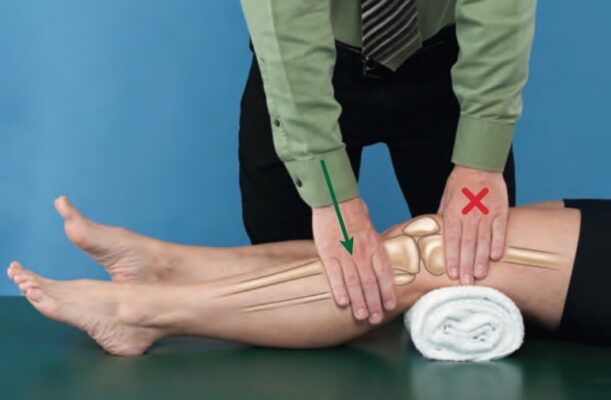
- Supine with knee in open-packed position & bolster or wedge just proximal to knee
- May be pre-positioned in varying degrees of flex to point of restriction
- Clinician position & Hand Placement:
- Stands on ipsilateral side
- Stabilizing contact: Hold distal femur against bolster or use pt’s body if the knee is flexed to >90°
- Mobilizing contact: Heel of hand contacts anterior aspect of proximal tibia
- Force Application:
- Apply force through your mobilization hand contact in a posterior direction that is parallel to the treatment plane of the joint.

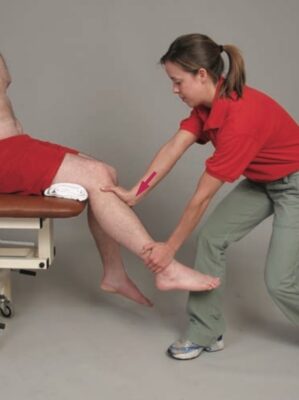
Accessory With Physiologic Motion Technique
- Patient Position:
- The patient is standing in an erect standing posture with his knees in extension.
- Clinician position & Hand Placement:
- You are in a lunge position behind the patient.
- The mobilization belt is positioned over the anterior aspect of the patient’s proximal tibia and around your leg. Both hands are used to stabilize and control motion into knee flexion.
- Force Application:
- The patient actively performs a squat moving the knee into flexion as you apply a posterior glide through the mobilization belt as the femur is stabilized.
- Mobilization force is maintained throughout the entire range of motion and sustained at end range.

Tibiofemoral Anterior Glide of Medial or Lateral Tibial Condyle
Indications:
- Anterior glide of medial tibial condyle is to improve tibial ER & knee ext
- Anterior glide of lateral condyle is to improve tibial IR & knee flex
Accessory Motion Technique
- Patient Position:
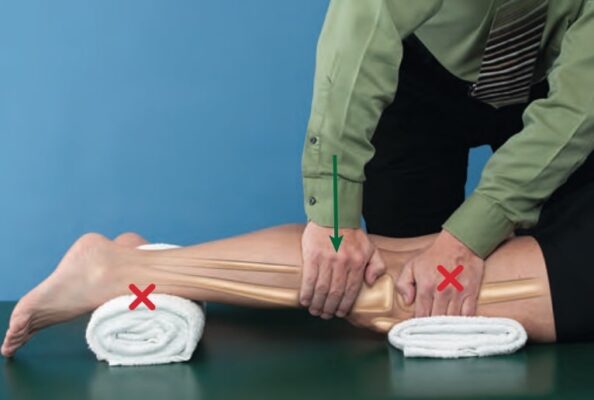
- Prone with knee in open-packed position & bolster or wedge just proximal to knee
- May be pre-positioned in varying degrees of flex to point of restriction.
- Clinician position & Hand Placement:
- Stands on ipsilateral side
- Stabilizing contact: Hand placed just proximal to ankle, providing counterforce to maintain knee position, or stabilization provided by placing lower leg on clinician’s shoulder if knee flexed >90°
- Mobilizing contact: Heel of hand contacts posterior aspect of proximal medial or lateral tibial condyle just below knee with forearm in direction of force or both hands contact proximal tibia if knee flexed >90°.
- Force Application:
- Apply force through your mobilization hand contact in an anterior direction that is parallel to the treatment plane of the joint.
- If both hands are used, one hand may provide mobilizing force anteriorly while the other hand provides posteriorly directed force as if opening a screw-top lid.
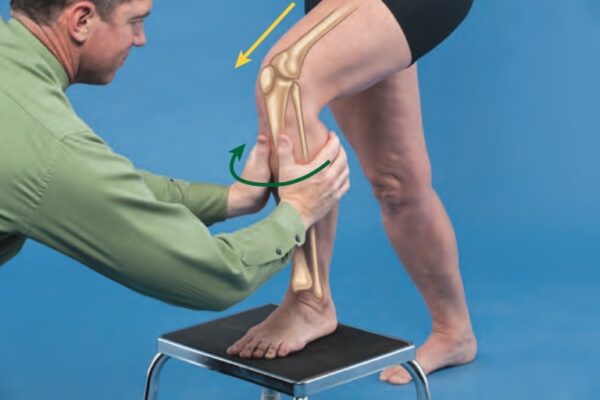
Accessory With Physiologic Motion Technique
- Patient Position:
- Stand in a lunge position with his or her involved foot placed on a stool.
- Clinician position & Hand Placement:
- You are half-kneeling facing the patient.
- Place one hand over the proximal medial tibial condyle and one hand over the proximal lateral tibial condyle and fibula just distal to the knee joint. Your forearms are in line with the direction in which force is applied, which varies during motion.
- Force Application:
- Apply an anteriorly directed force through the lateral tibial condyle and a posteriorly directed force through the medial tibial condyle as the patient lunges forward bringing the knee into greater ranges of flexion.
- Mobilization force is maintained throughout the entire range of motion and sustained at end range.
Tibiofemoral Posterior Glide of Medial or Lateral Tibial Condyle
Indications:
- Posterior glide of medial tibial condyle is to improve tibial IR & knee flex
- Posterior glide of lateral condyle is to improve tibial ER & knee ext
Accessory Motion Technique
- Patient Position:
- Supine with knee in open-packed position & bolster or wedge just proximal to knee
- May be pre-positioned in varying degrees of flex to point of restriction.
- Clinician position & Hand Placement:
- Stands on ipsilateral side
- Stabilizing contact: Hold distal femur against bolster or stabilization provided by pt’s body if knee flexed to >90°
- Mobilizing contact: Heel of hand contacts anterior aspect of proximal medial or lateral tibial condyle just below knee with forearm in direction of force or both hands contact proximal tibia if knee is flexed to >90°.
- Force Application:
- Apply force through your mobilization hand contact in a posterior direction that is parallel to the treatment plane of the joint.
- If both hands are used, one hand may provide mobilizing force posteriorly while the other hand provides anteriorly directed force as if opening a screw-top lid.
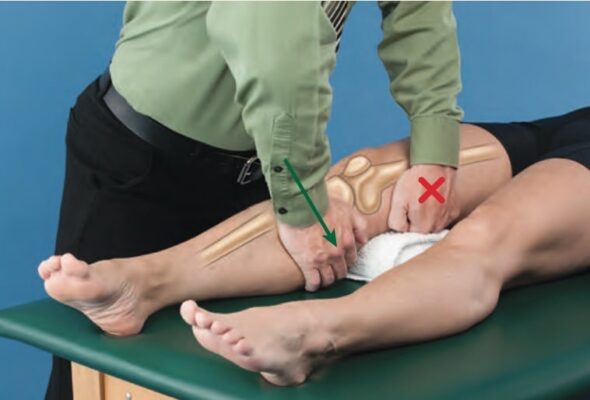
Accessory With Physiologic Motion Technique
- Patient Position:
- stand in a lunge position with the involved foot placed on a stool.
- Clinician position & Hand Placement:
- half-kneel facing the patient.
- Place one hand over the proximal medial tibial condyle and one hand over the proximal lateral tibial condyle and fibula just distal to the knee joint. Your forearms are in line with the direction in which force is applied, which varies during motion.
- Force Application:
- Apply a posteriorly directed force through the lateral tibial condyle and an anteriorly directed force through the medial tibial condyle as the patient extends the knee and steps up onto the stool.
- Mobilization force is maintained throughout the entire range of motion and sustained at end range.
PROXIMAL TIBIOFIBULAR JOINT MOBILIZATIONS
Proximal Tibiofibular Anterior and Posterior Glide
Indications:
- Anterior fibular & posterior tibial glide to improve knee flex
- Posterior fibular & anterior tibial glide to improve knee ext
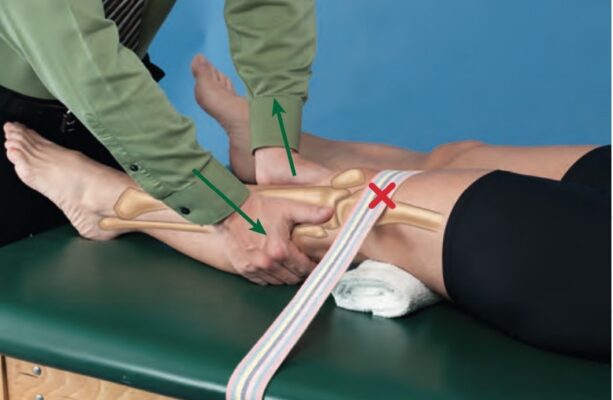
Accessory Motion Technique
- Patient Position:
- supine position with the knee in the open-packed position and a bolster or wedge just proximal to the knee.
- May be pre-positioned the knee in varying degrees of flexion to the point of restriction.
- Clinician position & Hand Placement:
- Stands on ipsilateral side
- Stabilizing contact: Hold distal femur against the bolster with belt
- Mobilizing contact: For anterolateral mobilization, fingers grasp posterior aspect of proximal fibular head with forearm in direction of force; for posteromedial mobilization, heel of hand contacts anterior aspect of proximal fibular head with forearm in direction of force
- Force Application:
- One mobilizing hand exerts an anterolaterally directed force to fibular head with posteromedial force to tibia through other mobilizing hand for flex
- One mobilizing hand exerts posterolaterally directed force to fibular head with anteromedial force to tibia through other mobilizing hand for ext
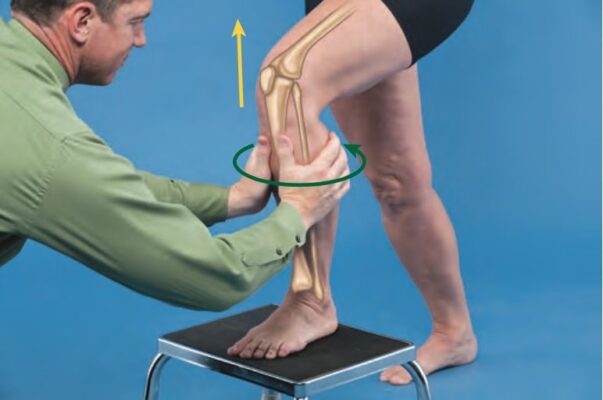
Accessory With Physiologic Motion Technique
- Patient Position:
- stand in a lunge position with the involved foot placed on a stool.
- Clinician position & Hand Placement:
- half-kneel facing the patient
- Place one hand over the proximal tibia and one hand over the fibula just distal to the knee joint. Your forearms are in line with the direction in which force is applied, which varies during motion.
- Force Application:
- Using both hand contacts, apply an anteriorly directed force through the fibular contact and posteriorly directed force through the tibial contact as the patient lunges forward bringing the knee into greater ranges of flexion.
- The patient may also step up onto the stool bringing the knee into greater ranges of knee extension as anteriorly directed force through the tibial contact and posteriorly directed force through the fibular contact is applied.
- Mobilization force is maintained throughout the entire range of motion and sustained at end range.
Tibiofemoral Flexion High-Velocity Thrust
Indications:
- To improve motion or reduce symptoms associated with deficits in knee flex ROM
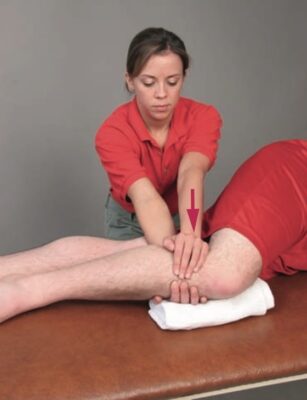
Technique:
- Patient Position:
- Supine with knee in flex & foot supported by clinician.
- Clinician position & Hand Placement:
- Stands on ipsilateral side
- Stabilizing contact: Fingers placed within popliteal crease to form fulcrum & grasp posterior aspect of tibia & fibula
- Mobilizing contact: Grasp distal lower leg just proximal to ankle
- Force Application:
- As your stabilization hand maintains the fulcrum, your mobilization hand flexes the patient’s knee to its maximum available range.
- Once resistance is engaged at end range, apply a high-velocity low-amplitude thrust by moving the patient’s knee into further degrees of flexion against the fulcrum of your stabilization hand.
References:
- Christopher H. Wise, Dawn T. Gulick. Mobilization Notes: Rehabilitation Specialist’s Pocket Guide. F. A. Davis Company, 2009.
- Christopher H. Wise. Orthopaedic Manual Physical Therapy: FROM ART TO EVIDENCE. F. A. Davis Company. 2015.
- Carolyn Kisner, Lynn Allen Colby, John Borstad. Therapeutic exercise : foundations and techniques, Seventh edition. F.A. Davis Company. 2018